From Oocyte to Embryo: Behind the Scenes in the Fertility Lab
With Jason Au - Embryologist, B.Sc., M.Sc.
With increasing awareness of how many Canadians are affected by infertility, more and more people are researching and pursuing fertility treatment. Of course, there are lots of questions. We'd like to share a look at what our scientists do to help individuals and couples achieve successful pregnancies.
Jason Au is one of five embryologists on the PCRM team. He attended the Canadian Fertility and Andrology Society conference in October, 2015, to present his findings from exciting research on better methods for determining embryo quality.
Jason's daily work in the lab includes retrieval of the gametes (sex cells – the oocyte and sperm), embryo creation, embryo culture, and selection of the best embryo(s) for embryo transfer. Let's take a closer look at what that entails.

Oocyte Retrieval
Oocyte maturation doesn’t begin with the oocyte retrieval, but actually much earlier with ovarian stimulation. At an injection teaching, patients meet with a fertility nurse to learn how to administer injectable medications, review their treatment schedule, and are encouraged to ask questions.
During fertility treatment, patients take medication to stimulate the ovaries and promote follicular growth. At this time, they visit the clinic for frequent ultrasounds and blood evaluations to monitor the response to the medications - and to determine the optimal time for the oocyte retrieval procedure.
When the oocytes are ready to be retrieved from the body, the follicular fluid is aspirated by a doctor and passed to the embryologist to be examined under the microscope. The retrieval is performed under sedation to ease the patient’s discomfort. The oocytes are then retrieved from the fluid. The retrieved ooctyes will be cultured until the insemination or injection later in the afternoon.
On the same day of the oocyte retrieval, a semen sample is collected from the partner or donor sperm is prepared for insemination. The sperm sample undergoes a wash to isolate the population of sperm with the best motility and morphology for insemination or injection.
Collection is generally non-invasive, unless the male patient is diagnosed with severe oligospermia or azoospermia. In these cases, surgical sperm retrieval from the testes may still be able to yield an adequate amount of sperm for fertilization. PCRM has two affiliated urologists who can provide consultation, as well as surgery, for patients with urological conditions.
Fertilization
Fertilization occurs in the lab through one of two processes:
1. In Vitro Fertilization (IVF): the sperm and oocytes are cultured overnight in a petri dish.
1. Intra-Cytoplasmic Sperm Injection (ICSI): a single sperm is selected and injected directly into the oocyte.
The recommended method of fertilization is based on the sperm parameters determined during a sperm functional analysis.
Signs of fertilization begin to show 15-18 hours after insemination/injection, making the timing of procedures extremely important. Procedures are carefully scheduled to allow embryologists to be on site to monitor the development of the embryos.
Embryo Culture and Selection
Once fertilized, embryos are cultured in the lab for six days.
Day 1: Fertilization check. The embryologist looks for two pronuclei in each embryo, indicating a normal fertilization.
Day 2: The embryos should begin to divide and reach the 2- to 4-cell stage.
Day 3: The embryos should continue to increase in cell number and reach the 6- to 10-cell stage.
Day 4: The embryos should have more than 10 cells and compaction should follow. This is when individual cells in embryos start to pack tightly together, forming a “morula” or solid ball of cells.
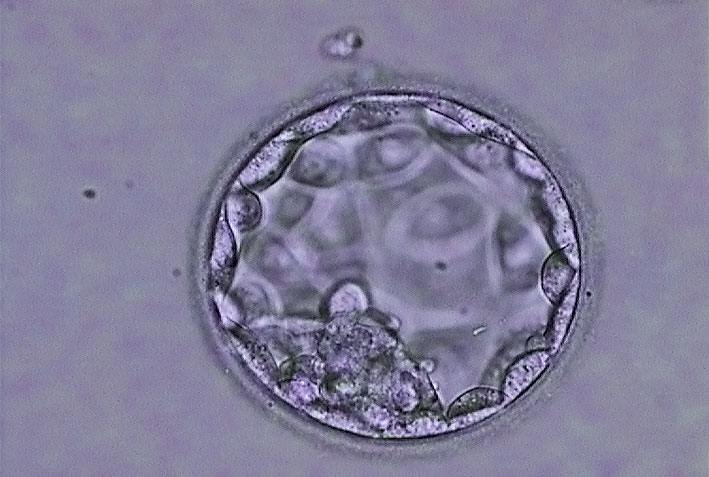
Day 5: The morula starts forming a fluid-filled cavity and cells differentiate into inner cell mass (ICM) and trophectoderm cells (TE) resulting in a blastocyst. Day 5 is typically when embryo transfer is performed. Embryologists will select the best embryo(s) based on morphology for implantation.
Day 5-6: After the top quality embryo(s) has been transferred, any surplus blastocysts that are of good quality will be cryopreserved. Currently, PCRM employs the vitrification technique for embryo cryopreservation. These surplus embryos will be kept safely at PCRM until patients desire to use them for a future cycle.
Patient Care
Patients first meet with Jason and the other embryologists on the day of oocyte retrieval. Each day that the embryos are in the lab, our embryologists contact patients to provide embryo updates —how they are developing, their quality based on morphology, and when the embryo transfer will take place.
On the day of the embryo transfer, the embryologist meets with the patient in the pre-operative area to do a final review, going over the grading of the embryos and confirming the number of embryos patients wish to transfer. The day after the transfer, our patients receive a final call from the lab to discuss how many remaining embryos are good quality and suitable for cryopreservation.
At PCRM we make it a priority to provide each patient with personalized support and care. We strive to create a calm and relaxing experience for everyone who is treated by our team.
Related Posts
Categories
About the PCRM Blog
Welcome to the Pacific Fertility Centre for Reproductive Medicine Blog! Nationally and internationally recognized for providing exceptional reproductive care, our team believes in empowering people with the knowledge they need to navigate their unique fertility journeys.
From information on the latest fertility treatments to valuable insights on egg donation, surrogacy, and everything in between, the Pacific Centre for Reproductive Medicine Blog is your ultimate resource for all things reproductive care and support. Read on to learn more, and contact us today if you have any questions or want to schedule a new patient appointment.

